From the George Washington University School of Public Health.
In 2013 a report in the Journal of Patient Safety stated that preventable medical errors that occur in hospitals are the third leading cause of death in America after heart disease and cancer. But hospitals and doctors will not discuss medical errors or advise patients how they can protect themselves. And the U.S. government does not recognize medical errors as a cause of death.
- Up to 3.65 million people will become victims of preventable medical errors.
- Over 1 million will be harmed (more than 2,700 a day).
- Up to 440,000 will die (more than 1,200 a day).
- At a total cost of approximately $1 trillion. In 2015 the U.S. military budget was $598 billion.
The April 2011 edition of the journal Health Affairs found that medical errors and other “adverse events” are rampant. This study found that mistakes occur in one out of every three hospital admissions. And these errors didn’t occur in mediocre hospitals, either. The study involved three high-quality teaching hospitals that were not named but were described as having “advanced patient safety programs, initiatives, and research projects.”
> An App is Helping Hospital Patients Protect Themselves
An investigation by the Office of Inspector General, Department of Health and Human Services released January 6, 2012 found that most errors are not reported and even in the case of errors that are reported and investigated changes are seldom made which would prevent them in the future.
Here are the categories under which serious reportable events (SRE) fall according to the National Quality Forum:
- Surgical or invasive procedure events
- Product or device events
- Patient protection events
- Care management events
- Environmental events
- Radiologic events
- Potential criminal events
Why is such a list important?
It is actually used to command quality from those who deliver healthcare to Americans. For example, Medicare, Medicaid and some private insurers will not reimburse doctors or facilities when one of their patients is a victim of an SRE. The Joint Commission, which is the accreditation body used by most U.S. hospitals, takes reported SREs into account when reviewing the facility for its updated accreditation. According to the NQF, as of 2011, about half of all states use the SRE list to assess the quality of their healthcare facilities, too. Patients benefit in two important ways from the SRE list: We know what medical mistakes and events we need to try to prevent on our own. The list of SREs is a list of unacceptable outcomes, one that helps us determine what preventive measures we need to take and one that outlines which ones might result in a lawsuit. When payers refuse to pay providers for making these mistakes, that puts the pressure on providers to figure out how to avoid adverse events. That can contribute to a safer environment for patients.
> An App is Helping Hospital Patients Protect Themselves
But there are also problems with the list: As in the past, the current list of never events or serious reportable events does not mention some medical errors that are just as devastating to patients, such as:
– Healthcare-acquired infections
– Missed diagnoses, misdiagnosis or lack of diagnosis
– Lack of follow up – post-hospital discharge or unreported test results that result in harm
If a provider knows they won’t be reimbursed because a serious reportable event took place they may try to cover up the event that does occur. Patients report having suffered these events only to learn later that their records have been amended, actual events have been removed from the records and that their only recourse is to deal with the facility’s risk management department, whose job is to protect the hospital from lawsuits. At that point they have no choice but to contact a lawyer for help.
Types of Preventable Medical Errors
Diagnostic
Error or delay in diagnosis
Failure to employ indicated tests
Use of outmoded tests or therapy
Failure to act on results of monitoring or testing
Treatment
Error in the performance of an operation, procedure, or test
Error in administering the treatment
Error in the dose or method of using a drug
Avoidable delay in treatment or in responding to an abnormal test
Inappropriate (not indicated) care
Preventive
Failure to provide prophylactic treatment
Inadequate monitoring or follow-up of treatment
Other
Failure of communication
Equipment failure
Other system failure
> An App is Helping Hospital Patients Protect Themselves
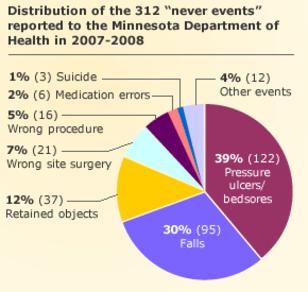
Some examples of preventable medical errors:
- Unnecessary surgery
- Surgery on the wrong person or body part
- Wrong procedure
- Surgical instruments and sponges left in bodies
- Undue Exposure to Radiation – i.e. unnecessary CT scans leading to development of cancer
- Medication errors
- Healthcare associated infections – i.e Clostridium Difficile (C.Diff), MRSA, VRE, CRE, caused by unclean conditions, materials, equipment or instruments resulting in severe sepsis and septic shock that can lead to death
- Bedsores/pressure ulcers
- Medical device failures
- Patient falls
- Blood clots
- Failure to Rescue – i.e. in-hospital strokes that are not immediately diagnosed and treated
- Blood and imaging test mix-ups, mistakes and unreported test results
- Hospital acquired acute renal failure
- Airway safety failure
- Iatrogenic delirium (delirium caused by improper treatment, especially in the ICU)
- Procedural harm
- Lack of follow up – post-hospital discharge or unreported test results that result in harm
> An App is Helping Hospital Patients Protect Themselves
Not all harm caused by medical treatment is preventable or avoidable, such as harm that is caused by necessary treatment for which there is a known and quantifiable risk to the patient, even when protocols and guidelines are strictly adhered to. In addition a factor must be included for normal human error. However harm due to human error can largely be eliminated through the proper and effective utilization of controls, such as checklists, that are designed for just such a purpose.
Reference: httpss://mha.gwu.edu/blog-preventable-harm/

Leave a comment
You must be logged in to post a comment.